Vitamin D
Sources of Vitamin D
★Endogenous synthesis from skin(that’s why its called a hormone due to synthesise in the body)
★Food rich in vitamin D (egg yolk,cod liver oil,butter, any fat rich diet)
Function and metabolism
Vitamin D maintain serum calcium and phosphorus concentration that supports cellular processes, neuromuscular function and bone mineralization . Vitamin D does this by:
- increasing calcium absorption from intestine( duodenum maunly)
- Stimulation of calcium reabsorption from kidney(Distal renal tubules)
- Act on parathormone to control serum calcium concentration.
Vitamin D disorders
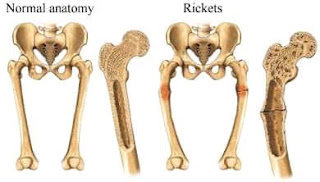
Rickets
Deficiency of vitamin D in growing children occrs due to imperfection of mineralization of bones and softening and destruction of the bones
Aetiology of vitmin D
- Prolong non exposure to sunlight
- Food deficient in vitamin D
- Kidney diseases( chronic kidney disease, renal tubular acidosis)
- Genetic disorders ( familial hypophosphatemic rickets, fancony syndrome, cystinosis)
- Malabsorption of vitamin D( liver and intestinal disorders)
Pathogenesis of rickets
Lack of Vitamin D
⏬
Inappropriate calcium-phosphate
⏬
homeostasis
⏬
Defective bone mineralization
⏬
Softening of the bones
⏬
Deformities and short stature
Clinical features
- Short stature
- protruded abdomen
- muscle weekness
- Box like head
- Delayed dentation
- dental carries
- poor enamel formation
- Pigeon chest deformities
- Harrison sulcus
- rachitic rosary
- Widening of wrist and ankle
- coxa vara and vulgus
- anterior bowing of leg
- gait deformities
- Tetany
- stridor due to laryngeal spasm
- Seizure
- Lordosis
- Scoliosis and
- Kyphosis
Investigation
Xray show
widening,cupping and frying of metaphysis wide gap between epiphysis and metaphysisdensity of Shaft reducedGreen stick fracture maybe present rachitic rosarycostrocondral ends of ribs ar expanded, cupped and indistinct
Blood picture
- Serum calcium (sc): usually normal
- Serum phosphorus (sp): low
Rachitic index( SC*SP)
Less than 30 :rickets likely
More than 40 :rickets unlikely
In between30-40 : doubtful
- Serum ALP: high
Serum PTH: high
Serum 25 (OH)D and 1,25 (OH)2D: low
Serum creatinine: high in CKD and RTA
Serum electrolyte: altered in CKD and RTA
Urine picture
- Urine for glucose : glycosuria(glucose present in urine)
- Urine for amino acid : aminoaciduria(amino acid present in urine) in fancony syndrome
- 24hour urinary calcium concentration: high in fancony syndrome
- Twenty four hour urinary phosphate concentration: high in RTA(road traffic accident) , X linked hypophosphatemic rickets and fancony syndrome, etc
Treatment
Vitamin D3 suppliment,
Calcium supplementation, and
Phosphorus supplimentation.
Prevention
1.Exposure to sunlight
2.Vitamin D and calcium rich food intake
3.Regular vitamin D intake
Osteomalacia
Deficiency of Vitamin D is the most common cause of osteomalacia in Adult. Vitamin D is an important nutrient that helps us absorb calcium ion in our intestine.
Certain conditions can interfere with the absorption of vitamin D and lead to Osteomalacia :
- Celiac disease an damage the lining epithelium of our intestines and prevent the absorption of many nutrients like vitamin D.
- cancer( some types) can interfere with vitamin D processing.
- Liver and kidney disease can affect the metabolism of vitamin D.
- A diet that doesn’t include phosphates can cause phosphate lower , which can lead to osteomalacia.
- Drugs induced osteomalacia: phenoytin phenobarbital etc
Sign and symptoms
- Bones fracture easily.
- muscle weakness
- hard time walking
- may develop a waddling gait.
- Bone pain, especially in hips, is also a common symptom.
- A dull, aching pain can spread from our hips to the lower back, pelvis, legs and ribs
very low levels of calcium in blood may causes :
- Arrhythmia or irregular heart beat
- Tingling and numbnes around the mouth and
- Tingling and numbness in the hands and feets.
- Spasms in hands and feets
Diagnosis of Osteomalacia :
- low levels of vitamin D
- low levels of calcium
- low levels of phosphorus
- Alkaline phosphatase is high (indicate Osteomalacia)
- Parathyroid hormone high (suggest lack of vitamin D)
- X ray show small cracks in bones(these cracks are called looser’s transformation zones. Fracture begin with this zone
Treatments of Osteomalacia :
- oral supplements of vitamin D, calcium, or phosphate for early detection
- Exposure to sunlight for Vitamin D production.
- Liver and kidney disease treatment prevent Osteomalacia due to liver and kidney disease can cause impairment of Vitamin D production.